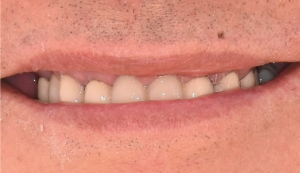
Pre-operative smile and orthopanthomogram. Fig. 1 (i, ii)

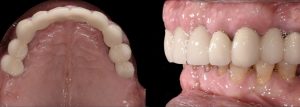
Occlusal and lateral view after periodontal treatment and extraction of tooth 16 and 28. Fig. 2
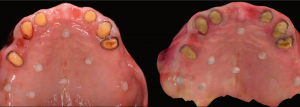
TIP: The accuracy of image registration between the CBCT and IOS scans can be improved with radiographic markers (composite blobs). Removing sources of radiographic scatter (in this case, the PFM bridge) also improves the accuracy. Fig. 3
The use of radiographic reference markers: a composite such as G-ænial Universal Injectable with a radiopacity of 250% Al, does not result in radiographic scattering during CBCT scans.

Prior removal of the porcelain-fused-to-metal (PFM) bridge: reduction of radiographic scatter caused by the metallic components of the prosthesis Intraoral surface scans (IOS) before and after removal of the original PFM bridge superimposed on the CBCT scan: this facilitates the planning of implant placement from a restorative perspective (restoration driven implant placement). (3Shape Implant Studio software) Fig. 4 (i, ii)
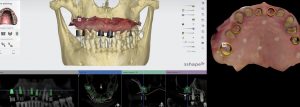
Planning of implant placement. A surgical guide is designed based on the desired implant position. (3Shape Implant Studio software) Fig. 5

Five implant fixtures were placed using a fully guided surgical protocol. Fig. 6

Flap raised in the 11 region as buccal bone grafting was required due to a bony defect. Fig. 7

Immediate post-operative following guided implant surgery and temporary cementation of the provisional fixed bridge printed from the GC Temp PRINT (medium shade). Fig.8

During the healing phase, tooth 24 developed pulpal necrosis and was endodontically treated. Fig. 9
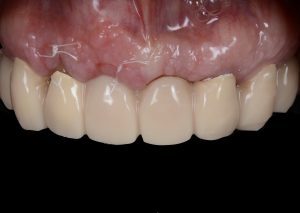
View at 10 days after implant surgery. Fig. 10

Pre- operative surface scan. Fig.11
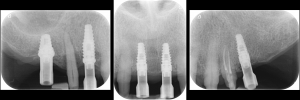
Periapical radiographs to verify the seat of the digital scan bodies. Fig. 12

Second set of provisional restorations printed with GC Temp PRINT (medium shade) using the Asiga Max UV 3D printer. Fig. 13
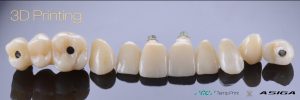
Completed provisional crowns, implant retained crowns and bridge, characterized with OPTIGLAZE color (GC) – Dental technician: Brad Groblar, Oral Dynamics, New Zealand. Fig. 14
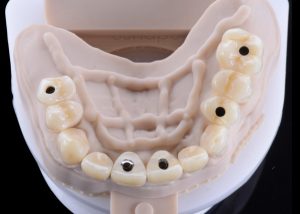
Completed provisionals fitted onto the printed models to allow the refinement of the contact points and occlusal contacts. Fig. 15 (i, ii)
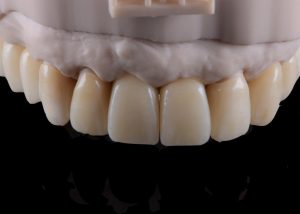
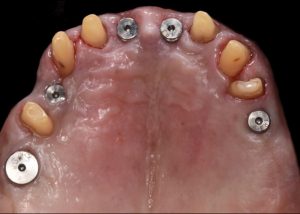
After removal of the temporary bridge from the first provisionalization phase. Tooth 15 was extracted. Fig 16 (i,ii)
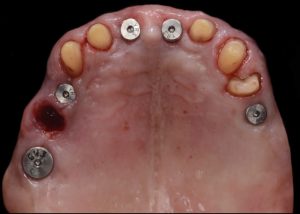
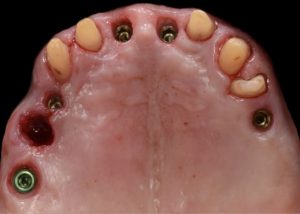
Healing abutments were removed and (b) the second set of temporary restorations was paced. Fig. 17 (i,ii)

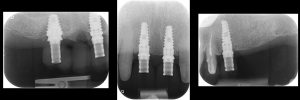
Periapical radiographs to verify the seat of the implant- retained provisional restorations. Fig. 18

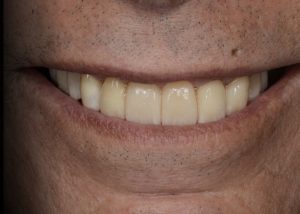
Immediate post-operative view of the inserted provisionals. Fig. 19 (i,ii)
Conclusion
Proper treatment planning protocols are the foundation of any fixed restorations in the arch involving dental implants. The data or information from the CBCT scan and intraoral surface scans (IOS) combined with the use of CAD software allow the simplification of workflows including diagnostic facially driven mock-ups, restoration-driven implant treatment planning and the design and fabrication of surgical guides.
The design of the temporary and permanent prosthesis and the design of the master die model can all be done on CAD software and then manufactured either with 3D printing or milling. The prosthetic design can be visualized, planned and even designed prior to the patient even attending for the surgical phase of treatment.
This case illustrates how advances in digital technologies can provide clinicians with the tools for diagnosis, treatment planning, the execution and provision of dental restorative procedures in a truly transformative way.
Simplification of clinical protocols, increased accuracy over conventional analogue techniques and improved patient comfort and outcomes are compelling reasons of the benefits of a full digital workflow in the field of restorative and implant dentistry.
About Dr. Anthony Mak
Dr. Anthony Mak obtained his dental degree at Sydney University (Australia) and then went on to complete his post-graduate diploma in Oral Implantology. He graduated with multiple awards and has worked with some of Sydney’s most renowned practitioners. His interests lie in dental technologies and advances in materials and techniques. He has a unique understanding in CAD/ CAM Digital dentistry and currently owns two practices in metropolitan Sydney focusing on comprehensive and implant dentistry.
Anthony has a thorough understanding of direct vs indirect dental restorations and has lectured internationally on the topics of Aesthetic and Digital Dentistry. He is a sought after speaker and is a key opinion leader for several global dental companies.
About Dr. Andrew Chio
Dr. Andrew Chio graduated as a dentist at the top of his year from the University of Melbourne (Australia) in 1995. On graduation he then undertook his dental internship at the Bendigo Base Hospital before spending the next one and a half years working in a rural hospital in Nepal.
He is the principle dentist of Arawatta Dental Centre in Carnegie and an active member of various dental associations. He is a lecturer and gives advanced hands-on trainings to dentists in specific areas of restorative dentistry.
About 3Shape
3Shape is changing dentistry together with dental professionals across the world by developing innovations that provide superior dental care for patients. Our portfolio of 3D scanners and CAD/CAM software solutions for the dental industry includes the multiple award-winning 3Shape TRIOS® intraoral scanner, the upcoming 3Shape X1® CBCT scanner, as well as market-leading scanning and design software solutions for both dental practices and labs.
Two graduate students founded 3Shape in Denmark’s capital in the year 2000. Today, 3Shape has over 1,500 employees serving customers in over 100 countries from 3Shape offices around the world. 3Shape’s products and innovations continue to challenge traditional methods, enabling dental professionals to treat more patients more effectively. www.3Shape.com




Comments are closed.